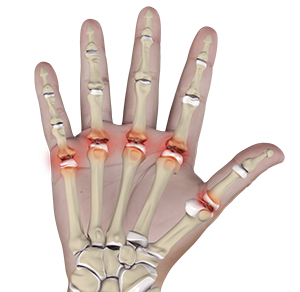
What is Metacarpophalangeal (MCP) Joint Arthritis?
The bones of the hand are called metacarpals and the bones of the fingers are called phalanges. The metacarpophalangeal joint or MP joint, also known as the first knuckle, is the large joint in the hand where the finger bones meet the hand bones. The MCP joint acts as a hinge joint and is important for gripping and pinching. When arthritis affects the MP joint, the condition is called MP joint arthritis. The condition is more common in the thumb joint and index finger joint.
Causes of Metacarpophalangeal (MCP) Joint Arthritis
Causes of MCP joint arthritis include but are not limited to:
- Inflammation (mainly rheumatoid arthritis)
- Traumatic injury leading to broken bone or loss of cartilage (Post-traumatic arthritis)
- Routine wear and tear of the MCP joint (osteoarthritis)
- Certain medical conditions (gout, pseudogout, psoriasis, etc.)
- Infections (after a cut, puncture or animal bite)
What are the Signs or Symptoms of Metacarpophalangeal (MCP) Joint Arthritis?
MCP joint arthritis can present with several symptoms such as:
- Pain that worsens during gripping and pinching activities
- Stiffness, swelling, deformity, and limited motion
- Feeling of weakness when trying to use the hand
- Shifting of fingers toward the pinkie (little finger) over time
- Joint pain at rest and at night in the advanced stages
- MCP joint that appears larger than normal
How is Metacarpophalangeal (MCP) Joint Arthritis Diagnosed?
Your doctor may evaluate the affected hand and MCP joint and assess for tenderness, range of motion, and stability of the joint. A plain X-ray or other imaging studies may be taken for further validation. Blood tests or imaging studies may also be ordered to fully confirm the diagnosis.
How is Metacarpophalangeal (MCP) Joint Arthritis Treated?
Several nonsurgical treatment options are available and known to be effective in controlling symptoms of mild-to-moderate MCP joint arthritis. However, the appropriate treatment depends on the amount of pain and loss of function. They include:
- Activity modification or hand therapy
- Anti-inflammatory medications
- Cortisone injections
- Simple splinting or flexible strapping
- Topical skin creams
If the condition is severe and nonsurgical treatments fail, your doctor may consider surgery. The optimal surgical procedure will depend on the type of arthritis, severity, and functional needs of the patient. The most common surgical options can be any of the following.
- Arthroplasty: Joint or bone replacement with silastic hinged or silicone or metal implants. This procedure is a popular option for fingers except for the thumb.
- Arthrodesis: This involves surgical fusion of the knuckle bones and immobilization of the joint. It is a reliable procedure to eliminate pain.
Synovectomy: The inflamed joint lining (synovial tissue) is removed (either with an open incision or arthroscopically) and the extensor tendons may be realigned.
Related Topics
- Wrist Fracture
- Fractures of the Hand and Fingers
- Wrist Sprain
- Flexor Tendon Injuries
- Distal Radioulnar Joint (DRUJ) Arthritis
- Ulnar Nerve Compression in Guyon's Canal
- Scaphoid Facture
- Industrial Hand Trauma
- Distal Radius Osteotomy to Correct Mal-Union (Crooked Painful Wrist)
- Distal Intersection Syndrome
- Distal Biceps Avulsion
- Adult Forearm Fractures
- Arthritis of the Hand and Wrist
- Arthritis of the Thumb
- Ganglion Cyst
- Boutonniere Deformity
- Carpal Tunnel Syndrome
- De Quervain's Tendinosis
- Dupuytren's Contracture
- Hand Pain
- Hand Infections
- Trapeziometacarpal (TMC) Arthritis
- Wrist Injuries
- Wrist Tumors
- Boxer's Fracture
- Swan Neck Deformity
- Carpal Instability
- Bennett's Fracture
- Kienbock's Disease
- Scapholunate Dissociation
- Triscaphoid Joint Arthritis
- Ulnar Carpal Impaction
- Triangular Fibrocartilage Complex Injury (TFCC)
- Guyon's Canal Syndrome
- Hand Masses
- Distal Radioulnar Joint (DRUJ) Instability
- Work Related Hand Injuries
- Wrist Ligament Tear and Instability
- Metacarpophalangeal Joint Arthritis





